The link between The Gut Microbiome and Mental Health Disorders
Science has shown that, through studying the gut-brain axis, we can draw clear links between our mental wellbeing and the state of our gut. Patients, on an individual level, are also able to help themselves by studying the signs and symptoms of gut-mental health. The management of gut microbiota has the potential to significantly improve a patient’s treatment outcomes.
The link between gut health and mental health has been explored extensively over the last decade. Clinical studies have grown a significant body of evidence suggesting that mental health and gut health are closely linked. This connection has been made through studying the gut-brain axis, whereby signals are sent from the gut (via the central nervous system) to the brain, bidirectionally.
Trials have been conducted in order to study this connection further. Mental health can pivot around the gut microbiota status, and can be linked to issues such as depression, anxiety, bipolar disorder, etc.
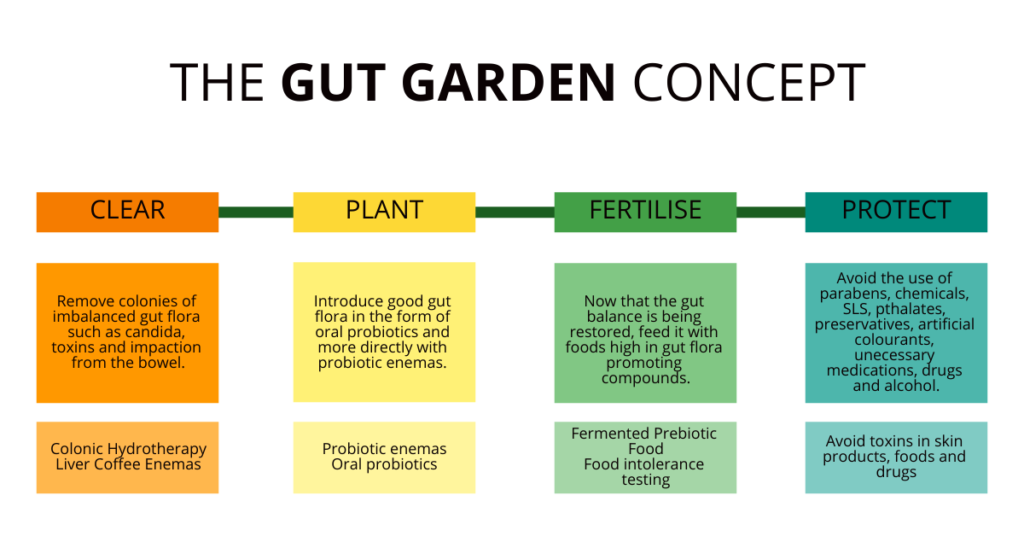
The Gut Garden Metaphor
Our gut can be compared to a garden. A garden is composed of thousands of small organisms that coexist to create balance in their ecosystems. This is very similar to our gut, where good bacteria help to fight off bad bacteria, improve immune function and digestive health. Now, think about a river that runs through this garden. This would be the vagus nerve that transmits signals to the brain. When our ecosystem is polluted, the river carries these bad “pollutants” (signals) to the brain, where our mental health is affected. The two are not mutually exclusive, and work together to provide balance to both ecosystems.
People who struggle with diseases like IBS (Irritable Bowel Syndrome), and Crohn’s Disease, share similar issues with their gut flora.
Mental Health, Probiotics and the Gut Garden
Clinical trials were conducted with a total of 1349 patients who suffered from mood disorders related to depression. Over the course of eight weeks, some patients were given a course of probiotics and others a placebo. It was found that those taking the real probiotic displayed huge improvements in cognitive functioning and depressive mood symptoms. Many more trials were conducted, with differing approaches, that all yielded positive results when using probiotics.
Many of us dismiss the powerful benefits of using probiotics in our everyday lives. A good probiotic consists of millions (if not billions) of live microbiota that help promote gut flora. By implementing a good quality probiotic into a patient’s life, they could see significant results in their pursuit for better physical and mental well being.
In extreme cases, clinicians can also refer their patients for faecal transplants. Faecal transplants involve transferring the stool of a healthy donor to the gastrointestinal tract of the diseased patient (usually those suffering with recurrent C. difficile colitis). Although the procedure may sound less than appealing, the results have been incredibly beneficial.
Summary
Science has shown that, through studying the gut-brain axis, we can draw clear links between our mental wellbeing and the state of our gut. Both systems coexist and work bidirectionally, and it is thus important to take care of them conjunctively. Integrative and Preventive Medicine is helping to equip health professionals in the pursuit of these treatment and prevention protocols. Patients, on an individual level, are also able to help themselves by studying the signs and symptoms of gut-mental health. The future of global health is improving significantly, thanks to the advancement of our understanding of the human body and the importance of gut health.
How do I Become a Functional Medicine Practitioner to learn more about The Gut and Mental Health?
The Institute of Integrative Medicine is a global leader in the field of Integrative Medicine Education. Integrative medicine aims to be at the forefront of modern technology and new discoveries. Understanding the link between the gut and mental health is essential. We offer certified online courses helping you to take charge of your practice and improve the quality of life for your patients. Find out more about the courses we offer today!
